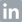What is Legionella?
Legionella is the genus of bacteria that causes Legionnaires’ disease, a potentially fatal form of pneumonia (lung infection), and the less severe, flu-like Pontiac fever, named for the Michigan town where it was first described. The former got its name from a pneumonia outbreak that occurred at an American Legion convention in Philadelphia in 1976, which infected over 180 people and resulted in at least 29 deaths. Legionnaires’ disease can also cause fever, cough, muscle pain and headaches.
How common is Legionnaire’s disease?
Incidents of Legionnaires’ disease have been rising steadily over the last two decades. Close to 10,000 people were diagnosed with the disease in the United States in 2018, though the CDC suggests the number of cases is likely much higher because many people with pneumonia are not tested for Legionella infection. About one in 10 people who gets sick from Legionnaires’ disease will die.
How is Legionnaires’ disease transmitted?
Legionellosis – also known as Legionnaire’s disease — is commonly contracted by inhaling water vapour containing the pathogen from sources like air conditioners, hot tubs or humidifiers. Legionellosis can present as either the flu-like Pontiac fever or the more serious and commonly–known Legionnaires’ disease. Legionella is not generally spread from one person to another.
Where is Legionella found?
Safe amounts of Legionella can be found in natural freshwater environments, like lakes and streams, but the bacteria can grow to dangerous levels in man-made water systems, including showerheads, cooling towers and plumbing systems. Cases have been linked to a variety of facility types, including hospitals, hotels, long-term care facilities and cruise ships. Mismanagement of these systems can put people at risk of contracting Legionnaires’ disease or Pontiac fever.
How does Legionella contamination happen?
Within a building’s water system, Legionella flourish within biofilms. Biofilms grow on the surface of infrastructure and consist of microorganisms stuck together with extracellular polymeric substances (EPS). They facilitate nutrient exchange, increase biocide resistance, protect against increased temperature and protect against shear stress. For instance, Legionella rely on other microorganisms within the biofilm to provide various required nutrients, such as the amino acid L-cysteine, that they cannot provide for themselves. This highlights the applicability of including general microbial monitoring in a Legionella monitoring plan.
Increased microbial risk and increased Legionella risk go hand-in-hand.
How is Legionella controlled?
Control measures for Legionella typically fall into three categories: temperature control (<20°C, >50°C), disinfection (oxidizing, non-oxidizing or UV) or point-of-use filtration. Which control strategy to use is highly dependent on the type of water system being managed. For instance, non-oxidizing biocides will not be used in a potable water supply.
In 2015, the American Society of Heating, Refrigerating and Air-Conditioning Engineers (ASHRAE) developed Standard 188: Legionellosis: Risk Management for Building Water Systems, which provides guidance on minimum Legionella risk management requirements for building water systems.
Learn why qPCR testing is a game changer for Legionella testing, and what the validation data has to say about its efficacy, benefits, and how it compares to other methods.
Who is susceptible to Legionnaires’ disease?
Anyone who is exposed to Legionella can contract Legionnaires’ disease or Pontiac fever but certain groups, including older people, smokers, those with weak immune systems or chronic lung diseases and those working in close proximity to large air-conditioning systems, are at higher risk.
Symptoms of Legionnaires’ disease typically develop two to 10 days after exposure to the bacteria. Those who develop pneumonia symptoms should see a doctor right away and be sure to mention any suspected exposure to Legionella. Symptoms of Pontiac fever can begin within a few hours to three days of exposure and usually last less than a week.
Facts and figures about Legionellosis
4% – The percentage that Legionnaires’ disease represents of all community-acquired pneumonias.
2 to 10 days – The typical incubation period for Legionnaires’ disease. In rare cases, it can take upwards of two weeks to develop.
2 to 48 hours – The typical incubation period for Pontiac fever.
35 degrees Celsius – The optimal water temperature for Legionella bacteria to grow.
Is Legionnaires’ disease contagious? – No. Legionella is not transmitted person to person.
Is there a vaccine for Legionnaires’ disease? – No. Legionnaires’ disease requires treatment with antibiotics. Pontiac fever is typically treated with rest and hydration but not antibiotics.